May 1, 2026
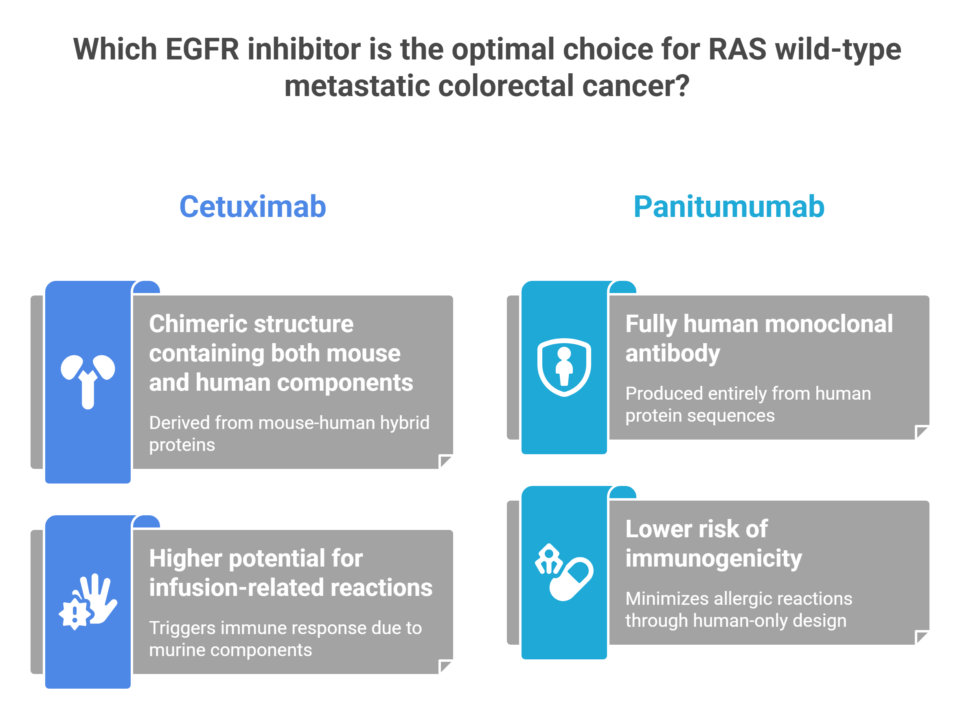
The story begins not in the clinic but in the molecular architecture of the drugs themselves. Cetuximab is a chimeric IgG1 monoclonal antibody — part mouse, part human. Its variable region, the targeting "head" of the molecule, is derived from murine cell lines. Panitumumab, by contrast, is a fully human IgG2 monoclonal antibody, produced through recombinant DNA technology so that not a single murine amino acid remains.