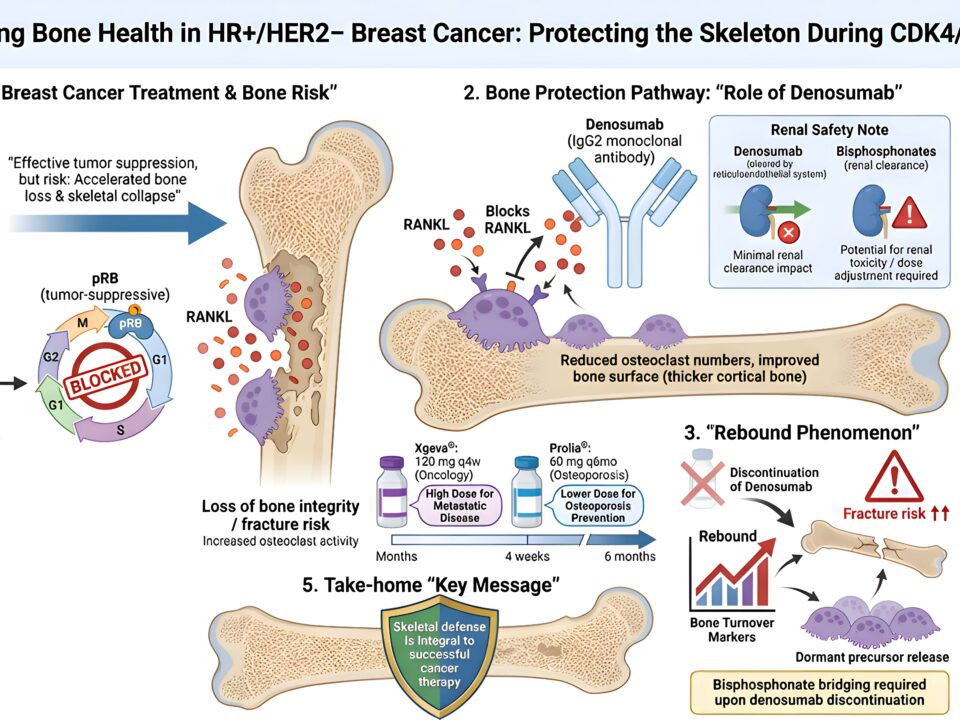
Choosing the right protein bag when prescribing TPN
February 18, 2022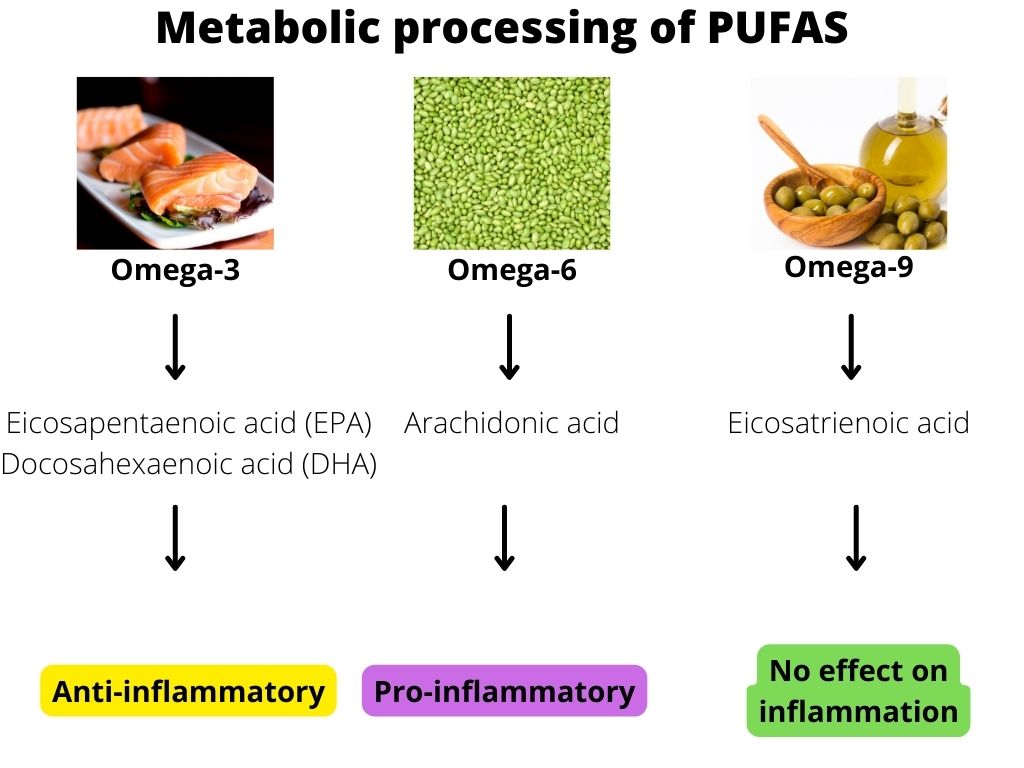
How to Start Immune Modulation by Nutrition?
February 27, 2022Supplemental parenteral nutrition
Supplemental parenteral nutrition, which we call SPN. And today the question is, does SPN really matter?
It is the addition of parenteral nutrition to enteral nutrition and all other nutrition to achieve nutritional goals that is calorie and protein targets. Whenever the patient is not able to meet more than 60% by enteral and all oral route.
SPN does not pose an infection risk. It can improve caloric and protein intakes, shorten the duration of mechanical ventilation, shorten the length of stay in ICU and in hospital.
SPN reduces the incidences of infection complications without apparent impact on blood lipids and sugar profiles or liver or kidney functions.
And after treatment, the albumin level was also significantly higher in the SPN group than in the enteral nutrition group. A significant cost reduction was found was SPN, suggesting that optimization of energy provision using SPN is a cost-effective strategy in selected critical ill adults.
The international guidelines recommend the use of SPN in cancer patients when they are malnourished and hyperphagia. And when enteral nutrition is not feasible.
In the same study, early seven-day SPN resulted in improved body composition, improved handgrip strength, improved serum pre-albumin levels in hyperphagia and hospitalized cancer patients at nutritional risk in the absence of any relevant clinical complications.
When is parenteral nutrition appropriate?
Consensus recommendations suggest:
- Initiating parenteral nutrition after seven days for well-nourished stable patients.
- within three to five days in those who are nutritionally at risk.
- And as soon as feasible in those with baseline moderate or severe malnutrition. If oral intake or enteral nutrition is not possible or sufficient.
- Critically ill obese patients may be a nutritionally at-risk population warranting earlier parenteral nutrition initiation.
SPN in COVID-19.
If a patient is on non-invasive positive pressure ventilation, they have no appetite. They can’t eat because the low oxygen levels, it is not possible to place a tube and then the only way to feed thing is to supply SIP feeds combined with SPN.
Regarding the gastric residual volume, there is no clear answer to this question. We cannot say don’t do GRV.
In the critical ill COVID patient it is safer to combine SPN with a lower volume of enteral nutrition to prevent aspiration. I did see aspiration in patients on full enteral nutrition that was COVID patients. Physicians always stresses that patient became hypermetabolic especially later in the disease. So, we should use you SPN to add up the shortage.
What is important when it comes to SPN?
It is the international recommendations on nutrition in the ICU should always be followed. Autophagy should be taken into consideration also in COVID-19 patients.
But let us use the results of the studies, feed our patients optimally and achieve good outcomes.
SPN Case study
Management of preoperative malnutrition by using SPN.
Patient is Mrs. DK, she’s a 59-year-old female. She had gastric bypass surgery 20 years ago, she’s on chronic hemodialysis. She was admitted with intermitted bowel obstruction and biliary colic. She had a total protein of 59, an albumin of 22 millimoles per liter, which is 2.2 grams per deciliter. Her appetite was healthy, and she was able to finish a proper meal.
But she presented with weakness. She couldn’t stand for more than 15 minutes and she had severe abdominal pain. So, the surgeon had to undo the bypass surgery.
She was referred for nutrition therapy was the instruction that the albumin should reach a level of 30 millimoles per liter and she should be in an acceptable nutritional condition prior to surgery.
I just want to mention this case is not about albumin it is about severe malnutrition. It is about the management of the patient and to get her in a better nutritional status prior to surgery and after surgery.
So, since she was eating fairly well and nutritional status and serum albumin is suspected to below due to previous bypass surgery, sub optimal absorption, chronic hemodialysis and insufficient dietary protein.
So, what approach would we use when we start SPN? Administer Albumin, supply a very high protein diet or prescribe high protein substrates?
Well, out of the history, we know that the only way to go was to start SPN. So, it was decided to supplement the intake with parenteral nutrition with the aim to improve her nutritional status parenteral nutrition was provided. It was 84 grams protein, 161 grams carbohydrate, 80 grams fat, 1769 kilo Cal and the rest of the protein the calories were provided by soft foods and semi elemental sip feed.
On day 8 preoperatively the surgeon had to decide about the surgery. The patient was feeling stronger and could walk further but the albumin was not at 30 and internist insisted that the albumin to be at 30 millimoles per liter. She said that the patient would die if we operate at that stage.
So, if a surgeon decided against the surgery, he gave another week to help improve her condition. And thus, intensifying the feeding strategy.
SPN continued and only used semi elemental sip feeds. On day 18. The surgeon argued that if he does not operate, she will die anyway because of the deteriorating condition of the gallbladder.
So, he decided to book the theater. on day 25 She was taken to theater. She survived surgery. She had a CRP of 283. On the day of the surgery, she was extremely ill.
And the surgeon’s preference for feeding was parenteral nutrition. Now between day 26 and a 72 There were many ups and downs A lot happened. Like desaturation, intubation, bowel distension, nausea and vomiting, diarrhea, no tolerance of enteral nutrition, CRP fluctuations, and she was extremely ill.
So parenteral nutrition was continued. A high nitrogen semi elemental feed was eventually started at 20 milliliter per hour. So SPN had to continue, micronutrients were also administered.
By day 73, the patient started slowly on a full fluid diet by day 75, the CRP was 82.5. We could stop all IV feeds, we continued enteral feeds, and a soft diet and renal friendly sip feeds were started.
On day 83, the patient was discharged from ICU and into the ward.
After total of 89 days in hospital she was discharged to a step-down facility on a renal friendly diet.
SPN nutrition therapy successful. So, there is a happy ending. Currently, she’s back to full time work with a good quality of life. So SBN was a lifesaver in this beautiful woman.